This March, AWD uplifts the Community Support and Health Services Domain of the Durham Comprehensive Aging Plan and Women’s History Month by focusing on an overlooked part of healthcare and community service – palliative and hospice care. One of the Community Support and Health Services goal is “support aging adults and their families in preparing for decisions about goals of care, including end-of-life care.”
As the Director of Special Projects in the Community Engagement Department at Transitions LifeCare, Betsy Barton’s focus is on educating marginalized communities about hospice and palliative care. She does this by building relationships, listening carefully, and respecting cultural mores and traditions. Betsy views death as a “constellation” created by the person with an illness, their friends, their family, their church – whoever is engaged with helping the person on their journey.
AWD spoke with Betsy Barton, a woman who is unafraid of tough conversations.

I was curious about your work with Transitions LifeCare. (Transitions LifeCare is for any stage of a person’s journey with a serious, or life-taking illness}
My job at Transitions is to reach out to underserved populations. That’s my entire job. I do have to do some bread and butter public presentations to other groups but really, almost everybody’s underserved. I want to focus on Black and African American, Latino & Hispanic, LGBTQ folks, Native American people. All are people who often don’t think that the medical community is hearing them, for instance, people with mental health issues. So many people. .
This is really fascinating, the work you do. What drew you to this?
I’ve really been involved in this work since I was about five years old, and that’s when my father first started to show symptoms of dementia. In a lot of ways, I’ve been a caretaker for sixty years. I’m sixty-five now, and in 1965 nobody knew what dementia was, or specifically frontal temporal lobe dementia. We assume now that he had it because others in my family ended up having it. I’ve always had, I guess I should say, a soft spot in my heart, for people with dementia.
I had an awareness of the struggles for people who had serious illnesses and the whole constellation around that. The person who has the illness and the caregiver and the kids, and the rest of the community who are around wondering what to do or just running the other way, saying, “I can’t deal.”
When you have that sort of illness, it impacts everything. As you just said, it impacts everyone in a relationship with that person.
Exactly. That’s the reason that I’m drawn to Transitions LifeCare because we look at the family as the unit of intervention. It’s the patient and the family, not just the patient, quote, “patient.” I hate that word, because you know, the person who is ill, it’s not just them in isolation. Our social workers work with the whole family. Our Transitions Kids Program works with the parents, the siblings who are going to survive, as well as the child who may die sooner rather than later. Or dealing with an ongoing long-term serious illness.
Plus my online passion for talking about taboo and unpopular health topics with vulnerable populations.
Say more please.
Throughout my whole life, that’s really what I focused on. I didn’t realize that at first. I just thought, “When am I going to realize what my mission is?” Then looking back, I realized, “Oh. This is what I’ve always done! Health-related adult education for people who are vulnerable. In my early years, I was working on rape awareness and violence against women, and then working with older folks. My first job out of college was working through Durham Tech as a contract employee teaching current events classes at local nursing homes.
Wow. That’s amazing.
Some of those places were pretty dire. And some of them were super-fun. I got to teach a class about North American Culture. I got a movie out from the library (there was internet in 1983) about making moonshine.

That’s so fun.
Yes, and they thought it was too. Then I worked on worker safety and health, and then peer education about HIV. I would say this is my happy place – talking about death and dying all day long. The ultimate thing that nobody wants to talk about.
Now I’m immersed in the cultural nuances of all the different ways that people don’t want to talk about it that are unique to their culture. It’s different in the Latino culture as compared to the Black and African American culture. And with white southern Baptists as opposed to the LGBTQ community: every group has their cultural take on that resistance.
That nuance. How do you learn the language of that?
I was fortunate to come in with a foot in many doors. When I worked in the area of workplace safety and health for nine years statewide, I met folks from literally every walk of life. Mostly working class folks, whether they worked in factories or they worked in the Imperial Foods chicken plant in Hamlet, North Carolina, which caused the deaths of 25 workers in 1991. The fire doors were locked, and they couldn’t get out.
Yes, I remember that.
Twenty five people died. Many others were seriously injured. I’ve been lucky to be a fly on the wall in many different places. Some of it is about intention. It’s about putting myself in those environments. For instance, on Saturday I went to the Islamic Association of Raleigh’s Open House. I’ve heard about it and was curious, so I went.
The big thing, I think, is caring. People are going to trust you if they can see that. The second thing is showing up. And maybe the third is not dominating, and being culturally humble.
What a great pair of words. Culturally humble. It sounds like this is an ongoing, exciting journey that you’re on, learning all these different cultures and how to be there for people. Whoever they are.
I think about ‘How do I need to present information that is important in a way it will be most heard and paid attention to?’ I’m very clear. I’m not attached to the outcome in terms of whether somebody may sign up for hospice or they might not, if they need it. That is their choice.
The important thing to me is that they know that they can, that they know it’s paid for by Medicare or Medicaid – a benefit they’ve usually already paid into – or most insurance. At Transitions LifeCare, we don’t turn anybody away for lack of ability to pay, even if someone’s uninsured.
That’s terrific.
Everyone should know that they have the right to be informed about the care options and then be able to access to them if they want to.
You mentioned marginalized communities. Can you speak about that a little bit? Like the intersections that suppress different communities’ access, and what that looks like when you’re facing illness or death. Or dementia.
It looks a lot of different ways. The data leads us to the more obvious places. For instance, if we look at African Americans as opposed to white people and the disparity between who signs up for hospice or how late they sign up, the disparities are huge. I would love it if I lived in the world where everybody signed up for hospice, or at least checked in about whether it would be good for them. People are eligible for hospice services at the point when a physician could answer ‘Yes’ to what they call the ‘surprise question’: Do I think this person is likely to still be alive in six months? Or stated differently, are they likely to die within six months?
We live in a culture where not even privileged white people necessarily sign up for hospice six months out to get that benefit. We’ve worked for it! But when we look at African Americans, as a group they use hospice less and they enroll later, which means they had all this time of suffering: five months, or five and a half months, or even five months and twenty-nine days. Literally, sometimes people die in the ambulance on the way to our impatient hospice.They could have gotten all this extra help and love and support.
What keeps people from coming earlier?

I think a lot of it is cultural taboos with that unique twist within each culture. Sometimes it’s health literacy. In some cultures it’s considered to be rude to ask the doctor a question. So, how are you even going to find out about something? If the physician or nurse practitioner, whoever the healthcare provider is, doesn’t mention it, you’re not going to know it’s an option. And they are often resistant.
That’s why we work with organizations like El Centro Hispano — to get that information out through Community Health Workers that support is available. And you don’t have to wait. Palliative care is not just for people who are dying. Palliative care is for anyone with a serious illness at any day or any stage who has bothersome symptoms. We can help with that.
And as you mentioned, because you are focused on marginalized communities, these are communities that struggle with the imposition of poverty, with redlining, with lack of access to medical care, or just a lack of trust, a learned and earned lack of trust, towards the medical community. As a queer person, I’m listening for cues all the time, right? At the doctor’s office: are you going to speak any of my language? Am I safe here?
Are you gonna use the word “homosexual?” I remember having a great conversation with my mentor at Duke, who is nationally known for her research. I said, “Well, you know, if someone uses the word homosexual, that’s how I know they’re not in my realm.” And she says, “What do you mean?!” (Laughs) So we had some great conversations back and forth about language, and how can tell a lot about a person by the terms that they use. She said “got it! I’m not going to say that any more.”
But you asked about disparities. In addition to the things that you mentioned, there is a bias that, is sometimes conscious and sometimes unconscious on the part of the provider or just the way our health care system is set up.
I had a conversation with a friend of mine about people in North Carolina and rural areas. I asked, “What do people do, who live out in the middle of the sticks and have all these barriers?” We just said, well, they die earlier. It doesn’t have to be that way. Things like health literacy, teaching. Getting people to know what their options are, getting them to know how to speak up, how to advocate for themselves and their family members. “Hey, I’d like to have a palliative peer consultation. I’d like to see if my loved one’s eligible for hospice.”
Our healthcare system is focused on the cure. We want to fix it.
There is a great book, Being Mortal, which is also a film. You can stream online for free. Great film. Great date night. (Laughter) But it is great. The focus is on healing an illness. We are more focused on healing the person and their family, given the circumstances that they have been dealt. That’s a different focus. Often that means when we have someone that we’re providing healthcare for, we might look at their pain management differently. We’re not worried about someone who’s at a very end of life becoming addicted to morphine.
There’s such a fear in our culture about becoming addicted to morphine. My supervisor says, “Tell me if you’ve ever taken oxycodone. Because if you have, you’ve already taken morphine.” It goes a long way to ease symptoms, easing pain, easing breath, shortness of breath, and even just relaxing, I would say, the soul – the soul and the body enough to make that transition, because there is a labor to death. Like there is a labor to birth.
With information and education, it’s not as scary.
You’re in Raleigh, is that right?
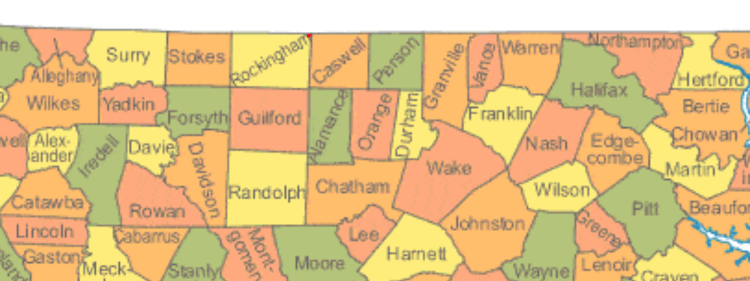
We actually cover ten counties. All the way out to Nash and Wilson and then out to Harnett and Johnson. Orange and Chatham, Franklin and Vance and Granville. And then Wake and Durham also. So ten counties. A lot of times people think we’re this tiny little organization. We’re not that tiny. Four hundred and fifty staff.
Wow.
Two hundred and fifty volunteers.
Who on any given day, are serving hundreds and hundreds of people. Six hundred people. Out in their home. Whatever they call home. A lot of times people think, well, I don’t want to go to a hospice. I want to stay home. Yes! Both and. It’s not an Either/Or situation. It’s Both/And.
I’m wondering how does the message get out, or how do we let our older community know that this is available?
Sometimes we get people interested by doing advanced care planning workshops. Or talking about the difference between hospice and palliative care. Because nobody’s heard of palliative care, or if they have, they think it’s equal to hospice, they think it means giving up. If they watch TV, like the New Amsterdam, there was a whole episode about the Palliative Care ward,” which makes no sense because your palliative care can be at home while you’re pursuing your chemotherapy. You don’t go somewhere to get palliative careandto get palliative care, and you don’t even have go to an inpatient hospice facility most of the time. You stay at home.
Sounds like a lot of education.
A lot of education and putting a little twist on that education to bring in a public health kind of perspective, which is my background. Tell me what you need to tell me, what you’re curious about. What do you want to know? Some of it is having people who are going to talk about these things that feel safe to the audience that we’re talking to.
How do you get your foot in the door of those different communities?
It’s all about relationships. We build relationships, and then build trust. Someone at first might think, “I don’t know who that lady is!” Then, by the end of an hour, we know each other. We see each other’s hurts. We’ve heard some of each other’s stories and the invitations just start happening.
Last week, I met three people for the first time and they asked, “Can you come to our church?” It was a Black church in Durham. “Can you come to our church and do what you just did over here in Cary?” Of course, the answer is, “Yes, yes I would.” It’s a classic “meeting people where they’re at.” People want to correct my grammar so they’ll say, “You mean meeting people where they are.” No, I mean it as they say in the Harm Reduction movement– we meet people where they’re at.
We created a video called “ An Act of Love” that’s narrated by Nnena Freelon. She’s a Durham-based jazz singer who’s a seven time Grammy nominee. When I heard she was writing a new book about grief (Beneath the Skin of Sorrow), I thought “We’ve got to get her for a book signing.” Now the book is written and tomorrow night she’s coming to Transitions and we have a sold-out crowd of a hundred and ten people signed up.
I’m so excited. She narrated this beautiful film that also has Bishop Clarence Laney in it who is a pastor from Durham. It interviews all Black and African-American, Latino, Hispanic, and rural folks. There are some queer folks in there too. Just talking about how “I didn’t know what hospice was,” people hearing from someone like them.
Every time I watch it, I’m always so happy because people just break into song at the end. There’s a death doula, Jennifer Evans, who sings and talks about singing someone out. Everybody breaks into song. Then the film ends with an upbeat kind of New Orleans jazz version of that song, and everybody starts singing and clapping.
It’s twenty-five minutes. It talks about the differences between hospice and palliative care, how important some advanced care planning is. I don’t talk at all. You hear me leading a workshop about healthcare planning, but there’s no interview with me. I created it. Found the funding, I produced it.
Wow! That’s incredible.

Is there anything else you want to leave us with?
One is to ask folks “Do you have your advance directive yet? Is it signed and legally valid in North Carolina?,” which means it is signed by two witnesses and you, and those signatures are all notarized.
Even if it’s too intimidating to do a whole advanced directive or living will, can you just name a healthcare proxy? And get that document signed, witnessed, and notarized. That’s an amazing first step, and you can always rip it up. You can always change your mind.
I’m doing an advanced care planning workshop in the Durham County Library on Monday, March 2nd from 5:30pm to 7pm. It’s interesting. It’s very interactive and dialogue based. It’s not a boring lawyer speaking at you! It’s very thought provoking and interactive.
There are so many people that need to know all of this.
Betsy Barton, MPH, CT
Betsy Barton is the Director of Special Projects in the Community Engagement Department at Transitions LifeCare in Raleigh. She plans and conducts interactive education on a variety of topics for clinical and community audiences.
Before coming to Transitions, she worked at the Duke Institute on Care at the End of Life, the Health Inequalities Program, and on Duke research teams related to serious illness, caregiver stress, medical decision-making, and race-based differences regarding decision-making at the end of life.
She has lived in Durham since 1978.





